Mental Health 101: Prevalence of Postpartum Depression
A (very brief) primer on depression during pregnancy & postpartum, & prevalence of postpartum depression across the globe
Mental Health 101 is an ongoing series where I discuss a mental health concern that is common throughout pregnancy or early parenthood. I started the series by covering “the baby blues.”
This week I talk a bit about depression during pregnancy and postpartum, including reviewing a meta-analysis that examined the prevalence of postpartum depression across 56 different countries.
Major depressive disorder is super common, whether you’re a parent or not. It’s estimated that 3-4% of the global population experiences depression and depression is the leading cause of disability worldwide. We often think of depression as feelings of sadness and emptiness, which it can be, but it can also involve irritability, anger, a lack of pleasure in things that used to bring you joy (known as anhedonia), and an inability to focus or concentrate. You can also experience physical symptoms, too, like extreme fatigue, difficulty sleeping (either sleeping too much or not enough), different eating habits (like eating too much or not enough), or body aches that can’t be explained by other conditions. Some people who experience depression might have suicidal thoughts or try to hurt themselves. Women are twice as likely to experience depression as men, and it’s possible that one contributing factor in this difference is the prevalence of depression during pregnancy and postpartum.
Depression that occurs during pregnancy is referred to by many names (antepartum depression, maternity depression, prenatal depression, perinatal depression) and affects about 10-25% of adult pregnant women1. Postpartum depression (i.e., a depressive episode occurring within one year of having a child) is about just as common, with many websites citing 10-15% prevalence rates for women.
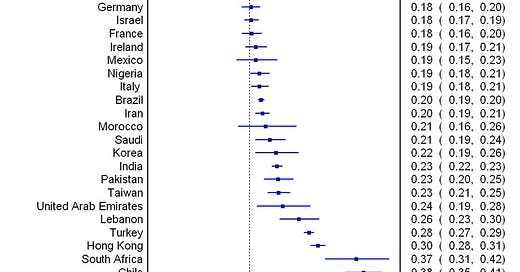
Hahn-Holbrook, Cornwell-Hinrichs, & Anaya (2018)2 conducted an extensive meta-analysis of prevalence of postpartum depression from 291 studies across 56 different countries. They found that the average prevalence globally was about 17.7%. However, there was a massive range in prevalence from country to country, from 2% prevalence of postpartum depression estimated from studies in Singapore to 38% in Chile, with studies from the United States estimating a 13% prevalence. See the graph below to view the prevalence rates from 40 of the countries that had studies on postpartum depression.
The authors were also interested in economic and health factors that contributed to higher versus lower rates of postpartum depression across countries. Nations with higher wealth inequality (as measured by the GINI index) and higher percentages of women working more than 40 hours per week had a higher prevalence of postpartum depression. Unsurprisingly, nations with a higher risk of maternal or infant mortality also had a higher prevalence of postpartum depression. National maternity leave policies3, cesarean section rates, percentage of infants born outside of marriage or living in single parent homes, and living in an urban environment were not significantly related to prevalence of postpartum depression across studies.
I was a little surprised at the finding that the percentage of women working full-time in a nation was related to postpartum depression prevalence. Obviously, this doesn’t mean that working full-time is bad for an individual woman’s mental health - these are national averages, after all, and it’s not accurate or useful to interpret the data this way. Rather, there are probably numerous underlying factors that contribute to national differences in the amount of women who work full-time that are affecting this relationship with postpartum depression. Indeed, the authors note that the rates of women working in a country were correlated with wealth inequality: Nations with more wealth inequality also had more women working full-time. This makes sense in that wealth inequality probably contributes to the differences between countries in how many women (particularly mothers) have to work for survival/financial necessity. Though speculative, my guess is that working for survival has more to do with mental health outcomes like postpartum depression in mothers than working in general.
The authors note that they obviously couldn’t examine all potential contributing factors to postpartum depression prevalence that may differ between countries. They also note that the majority of research on postpartum depression has been completed in Western countries (including 42 studies from the United States, 16 studies from the United Kingdom, and 23 studies from Australia that were analyzed), which make those national estimates more reliable than the estimates for countries with the fewest studies (e.g., there were only two studies from Mexico, two studies from Morocco, and three studies from Finland, not to mention the 16 countries that were only represented by one study and thus estimates for postpartum depression prevalence were not calculated). Overall, though, this is an incredibly comprehensive review of the literature (291 studies is A LOT to analyze) that gives us some valuable information about some systemic factors that may contribute to rates of postpartum depression worldwide.
Depression during pregnancy and postpartum is incredibly common. Because it’s so prevalent, there’s a lot to say about it. In fact, a Google Scholar search of “postpartum depression” brings up 409,000+ studies! Suffice it to say, one email newsletter is not enough to scratch the surface of the depth and breadth of research on depression throughout pregnancy and postpartum, including on its consequences for parents and children as well as effective treatments. Stay tuned for more.
Field, T. (2017). Prenatal depression risk factors, developmental effects and interventions: a review. Journal of Pregnancy and Child Health, 4(1). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5502770/
Hahn-Holbrook, J., Cornwell-Hinrichs, T., & Anaya, I. (2018). Economic and health predictors of national postpartum depression prevalence: a systematic review, meta-analysis, and meta-regression of 291 studies from 56 countries. Frontiers in Psychiatry, 8, 248. https://doi.org/10.3389/fpsyt.2017.00248
The authors don’t comment about this, but my hunch is that wealth inequality, women working full-time, and national maternity leave policies are all related to one another, so it would be hard to separate these factors from one another and their relationship to postpartum depression. I also think it might be more informative to look at how maternal leave policies affect mental health within a country (e.g., comparing the policies of one US state to another) versus between different countries.





not include all africa